X-Leg Treatment: What Is Genu Valgum and How Is It Corrected?
The treatment of knock knees, medically referred to as “genu valgum,” involves correcting the deformity where the knees touch but the ankles remain apart. This condition is not merely a cosmetic concern; it disrupts the load distribution across the knee joint, potentially threatening joint health over time. Particularly common in childhood, this condition is often considered physiological (normal) up to a certain age, but in older individuals or with severe angulation, it is regarded as pathological.
The mechanical axis distortion of the lower limb can cause excessive load on the outer knee compartment and strain the inner ligaments. Therefore, when planning treatment for knock knees, patient age, severity of deformity, and underlying causes must be carefully evaluated. This article is intended for informational purposes only and does not substitute professional medical advice; diagnosis and treatment should always be carried out by a qualified physician.
What Is Knock Knee (Genu Valgum)?
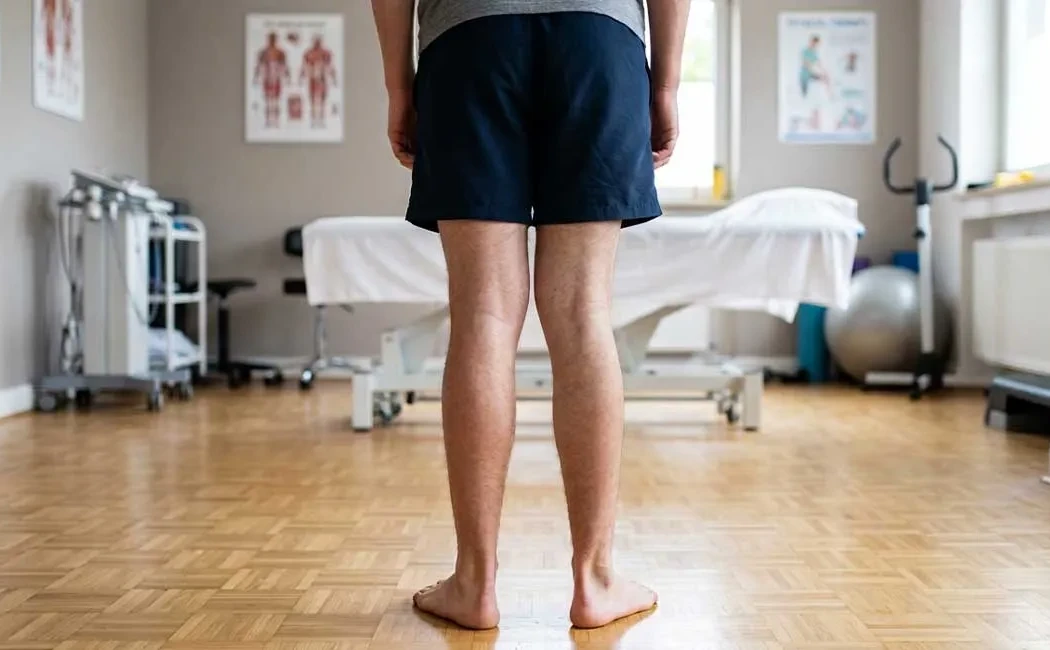
Genu valgum is characterized by the knees touching each other while there is a notable gap between the ankles when standing. In normal leg alignment, the mechanical axis runs through the centers of the hip, knee, and ankle in a straight line. In knock knees, this axis shifts outward, causing the knee joint to bend inward.
A mild knock knee appearance in children around ages 3-4 is considered normal growth-related and usually resolves spontaneously by ages 7-8. However, deformities that persist or arise during adolescence may require treatment. More detailed information on treatment of knock knees in children is important to understand approaches in the growing age group.
Causes of Knock Knee Deformity
A variety of factors contribute to the development of knock knee deformity, ranging from genetic predispositions to metabolic disorders. In some cases, the cause remains unknown (idiopathic), but accurate identification of underlying reasons directly affects treatment success.
Common causes include:
- Genetic Predisposition: Family history of similar deformities.
- Metabolic Bone Diseases: Conditions such as rickets (vitamin D deficiency) leading to bone softening.
- Trauma: Fractures or injuries affecting the growth plates around the knee.
- Infections: Bone infections (osteomyelitis) causing damage to the growth plate.
- Obesity: Excess weight increasing pressure on the knee joints.
These causes, especially in pediatric patients, fall under the scope of childhood lower limb deformities and can be managed effectively with early intervention. Additionally, congenital deformities treated surgically in children may also present as knock knees.
What Health Issues Can Knock Knees Cause?
Untreated severe genu valgum is more than a cosmetic problem; it’s a biomechanical disorder. Excessive load on the outer compartment of the knee can lead to cartilage wear and early osteoarthritis.
This uneven load distribution can trigger the following problems:
- Knee Pain: Especially in the front and outer parts of the knee after activity.
- Gait Disturbances: Knees knocking together while walking, causing balance issues.
- Meniscal Tears: Increased pressure on the lateral meniscus leading to tear risk.
- Patellar Problems: Tendencies for the kneecap (patella) to track outward.
Diagnostic Methods for Knock Knee Deformity
Diagnosis begins with a detailed physical examination. The physician observes the patient’s gait and measures the intermalleolar distance—the space between the ankles when the knees touch. Definitive diagnosis and evaluation require radiological imaging.
Typically, a full-length orthoroentgenogram is taken, showing the leg from hip to ankle. This X-ray helps calculate the mechanical axis deviation (MAD) and knee joint angles (LDFA, MPTA) to locate and quantify the deformity.
Treatment Options for Knock Knee
Treatment is personalized based on the patient’s age, cause, and severity of the deformity. Methods used in lower extremity deformity surgery range from non-surgical monitoring to complex bone correction procedures.
Non-Surgical Methods
In mild cases or children with remaining growth potential, non-surgical approaches are generally preferred initially.
- Observation and Monitoring: Regular follow-ups for cases within physiological limits.
- Medication: Vitamin D and calcium supplements for metabolic causes like rickets.
- Weight Management: Diet and exercise to reduce excessive joint load caused by obesity.
- Orthotic Devices: Occasionally used in selective cases for support.
Correction by Osteotomy
In adults with completed bone growth or adolescents with severe deformity, surgery is usually required for a permanent solution. Osteotomy involves controlled bone cutting to realign the angle. This procedure restores the mechanical axis of the leg to balance the load on the knee joint. It can be combined with bone lengthening and deformity correction surgeries and may sometimes be performed simultaneously with limb lengthening.
The Role of Osteotomy in Treating Knock Knees
Osteotomy is regarded as the gold standard surgical approach for knock knee correction. The primary goal is to delay or eliminate the need for knee replacement surgery. As one of the joint-preserving surgical techniques, osteotomy preserves the patient’s native joint.
Preoperative and Postoperative Procedures
Successful treatment relies as much on postoperative care as on preoperative planning. Measurements are meticulously made before surgery to prepare the patient. Postoperatively, the focus is on bone healing and regaining muscle strength.
Physical therapy is vital during recovery to maintain joint range of motion and strengthen muscles. Exercises aimed at preserving joint health can accelerate rehabilitation. Recovery timelines vary by individual but generally allow return to normal activities within a few months.
Risks and Complications in Knock Knee Treatment
As with any surgical procedure, knock knee correction surgeries carry certain risks. While an experienced surgical team and proper techniques reduce these risks, patient awareness is important. Potential complications include infection, nerve injury, and nonunion of the bone.
Additionally, occasional cases of malunion requiring revision surgery may occur. Managing these complications often requires advanced surgical expertise.
When applied appropriately and timely, knock knee treatment significantly improves patients’ quality of life and helps protect joint health.
The content, images, and information provided on this website are for general informational purposes only and do not constitute medical advice. The information presented cannot replace professional medical diagnosis, treatment, or consultation. If you have any health concerns or questions, please consult a qualified healthcare professional. This content reflects the views of Prof. Dr. Halil İbrahim Balcı; however, every patient's condition is unique, and treatment plans should be individualized.