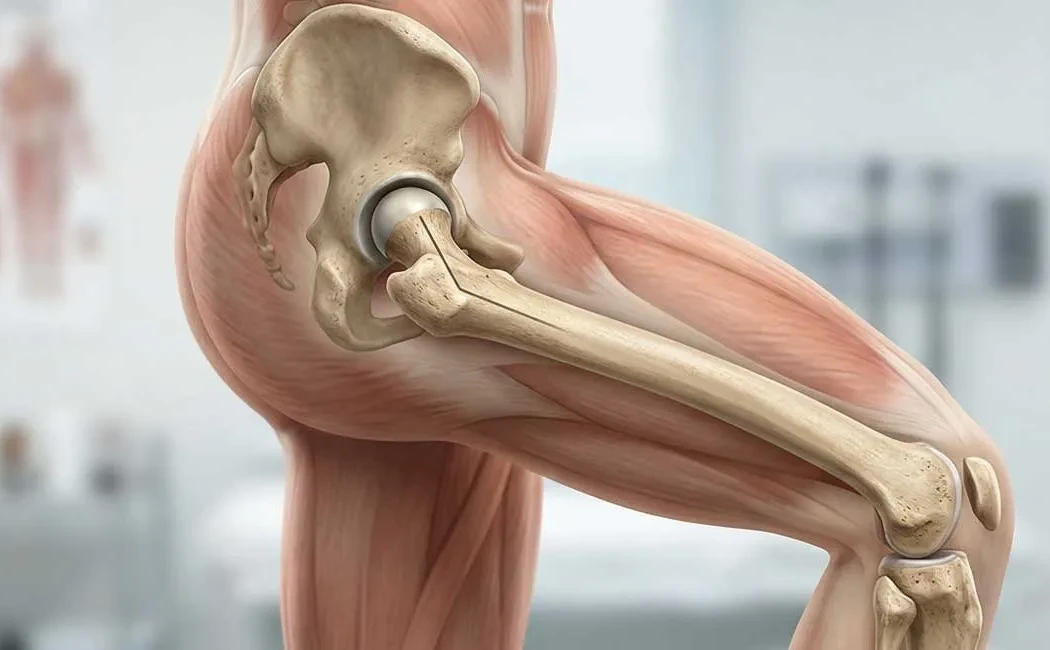
What Is Femoral Anteversion? Diagnosis and Surgical Treatments
Femoral anteversion is a common lower limb deformity where the neck of the femur (thigh bone) twists forward more than normal relative to its shaft. This anatomical variation causes the entire leg to rotate inward to fit the hip socket. Commonly referred to as “in-toeing,” this condition often manifests during early childhood with noticeable gait abnormalities and can be a significant concern for parents.
Although it often improves naturally with growth, excessive femoral anteversion can predispose individuals to hip and knee problems in adulthood. Diagnosis is confirmed through thorough clinical evaluation and radiological imaging. Treatment is tailored based on the severity of the deformity, patient age, and any functional impairments affecting daily life.
What Is Femoral Anteversion?
The femur is the body’s longest bone, extending from the hip to the knee. The angular relationship between the femoral neck and shaft directly influences leg positioning. Normally, infants are born with a degree of anteversion which decreases by around ages 8 to 10. When this angle remains above normal limits, it is defined as femoral anteversion.
This leads to the hip internally rotating to maintain joint stability. Consequently, the knees and feet point inward rather than straight ahead. The illustration below contrasts normal and anteverted femur positions.
Symptoms and Clinical Signs of Femoral Anteversion
The most obvious sign of femoral anteversion is inward-pointing toes during walking, commonly noticed when a child starts walking. Clinical observations and patient-reported symptoms include:
- In-toeing Gait: Inward rotation of feet and knees is the hallmark symptom.
- W Sitting: Children often sit with legs folded in a “W” shape, a common indicator due to the inward rotation of the hips.
- Frequent Tripping or Falling: Feet may catch on each other, causing balance issues and increased falls.
- Altered Running Pattern: A distinctive “egg-beater” running style with legs swinging outward may be observed.
- Hip and Knee Pain: In older children and adults, abnormal weight distribution may cause discomfort in the groin or around the knee.
Causes and Risk Factors of Femoral Anteversion
The exact cause of femoral anteversion is unclear but is believed to involve genetic factors and fetal positioning. It often runs in families; children with relatives affected have a higher chance of developing the condition.
It may also be associated with other childhood lower limb deformities. Children with a history of developmental hip dysplasia are at increased risk. Mechanical factors such as restricted fetal movement in the womb can influence bone development.
Rarely, neuromuscular disorders like cerebral palsy cause muscle imbalances leading to torsional deformities. Such complex cases require specialized assessment in the field of pediatric deformity surgery.
Diagnostic Methods
Diagnosis begins with a detailed physical examination. The physician assesses gait and measures hip rotation range of motion. The prone hip rotation test is particularly informative, with an increased angle of inward rotation relative to outward rotation supporting the diagnosis.
Imaging is essential for quantifying deformity severity and surgical planning. Below is a representative image of diagnostic imaging.
- X-rays: Evaluate the status of hip and knee joints.
- Computed Tomography (CT): Provides the most accurate measurement of femoral anteversion angle and allows three-dimensional bone assessment.
- Magnetic Resonance Imaging (MRI): Used when detailed evaluation of cartilage and soft tissues is necessary.
Treatment Options
Approach to femoral anteversion treatment varies according to patient age and deformity severity. Since spontaneous improvement is expected up to ages 8–10, observation is the initial strategy. Surgery is considered for persistent deformities causing functional problems.
Non-Surgical Methods
Mild to moderate cases, especially in growing children, are managed conservatively. These methods address symptoms and support natural correction rather than structural change.
- Observation and Monitoring: Regular check-ups to track angle changes.
- Adjusting Sitting Habits: Encouraging sitting cross-legged rather than in “W” position.
- Physical Therapy: Exercises to balance muscles and improve gait quality.
- Special Shoes and Insoles: Generally not effective in correcting the deformity but may aid in cases with flat feet.
Femoral Osteotomy and Surgical Approaches
If the condition does not improve after age 8–10, causes severe gait disruptions (frequent falls, difficulty running), or is cosmetically distressing, surgical treatment called “Derotational Femoral Osteotomy” is performed. This specialized procedure falls under lower extremity deformity surgery.
The surgery involves controlled cutting of the femur, rotating it to the correct angle, and stabilizing with plates, screws, or intramedullary nails. The main steps are illustrated below.
Osteotomy may be combined with bone lengthening surgery if there is leg length discrepancy, correcting both torsion and length in one procedure. In adults, it may be considered as part of joint-preserving surgeries aimed at delaying or preventing joint replacement.
The operation is performed under general anesthesia. Weight-bearing restrictions apply until bone healing is confirmed, typically with radiographic evidence after 6–8 weeks. Advanced deformity correction surgical techniques offer high success rates with manageable risks.
Post-Treatment Care and Follow-Up
The postoperative period is critically important. Recovery depends on the surgical method and bone quality. Rehabilitation generally starts within days after surgery.
- Hospital Stay: Typically 2–4 days of inpatient care.
- Weight Bearing: Partial weight-bearing with crutches or walker as advised by the surgeon. Full weight-bearing usually begins after radiographic evidence of bone healing.
- Physical Therapy: Intensive rehabilitation to maintain joint range and regain muscle strength.
Complications, although rare, can occur. Delayed or non-union of bone may require non-union surgery. Incorrect bone healing may necessitate revision surgery. Regular postoperative evaluations and imaging are essential. With successful surgery and rehabilitation, patients generally return to normal activities and sports.
The information provided herein is for general informational purposes only and does not constitute medical advice, diagnosis, or treatment. The diagnosis and treatment of femoral anteversion and other orthopedic conditions vary based on individual patient circumstances. For any health-related concerns or decisions regarding treatment, please consult a qualified healthcare professional. While the content is based on current scientific sources, medical practices may evolve over time. Do not delay seeking professional care based on this information.