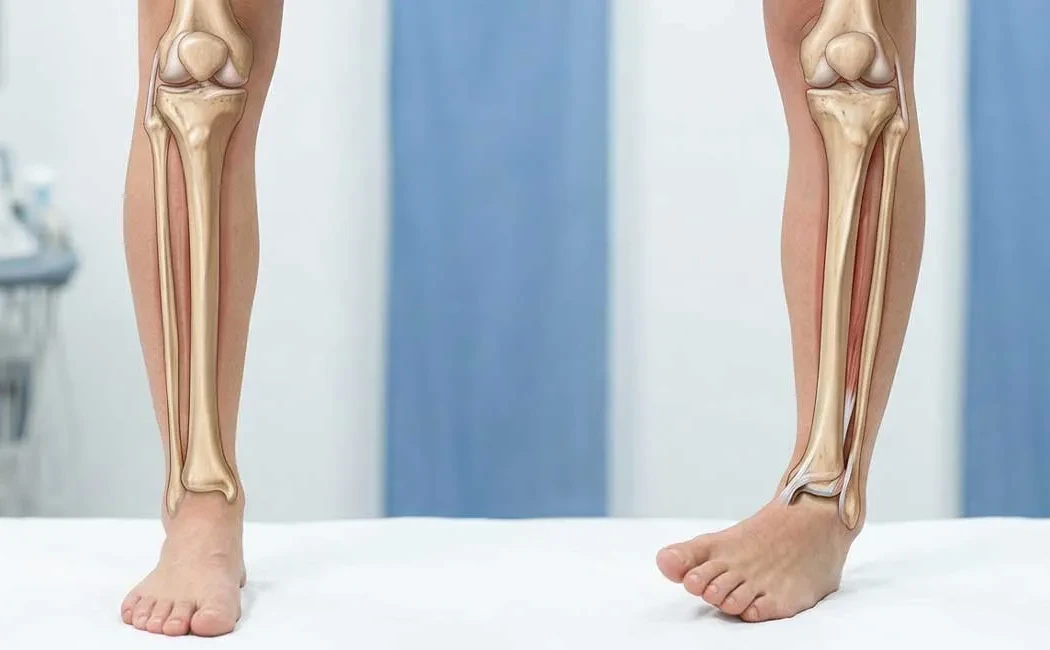
Rotational Deformity: Hidden Bone Twists and Diagnosis
Rotational deformity refers to the abnormal twisting of the long bones in the lower limb (femur or tibia) around their longitudinal axis. Commonly referred to as “bone twisting,” this condition may not always present as a visible deformity externally, yet it can significantly impact a patient’s gait pattern, joint biomechanics, and overall quality of life. It often manifests with knee cap and ankle pains, and if left undiagnosed, may lead to early joint degeneration.
This complex orthopedic issue can be congenital or develop following trauma with improper bone healing. Diagnosis requires advanced imaging techniques capable of capturing the three-dimensional bone structure beyond standard X-rays. Treatment ranges depending on deformity severity and symptoms, from physical therapy to complex reconstructive surgeries.
What is Rotational Deformity?
Rotational deformity is a torsional abnormality around the bone’s anatomical axis. It most commonly affects the femur (thigh bone) and tibia (shin bone). Normally, each person has a certain degree of natural torsion; however, when these angles exceed physiological limits, they are considered pathological.
This condition causes the leg to twist excessively inward or outward, altering foot positioning during walking. The diagram below illustrates various types of rotational deformities and their anatomical manifestations.
Common subtypes include femoral anteversion (inward twisting of the femur) and tibial torsion. These structural deviations disrupt load distribution across the hip, knee, and ankle joints, creating mechanical pain.
Causes and Risk Factors
The causes of rotational deformities are divided into two main groups: congenital (developmental) and acquired. Developmental deformities typically appear during childhood bone growth, with genetics playing a potential role. Some positional deformities in the womb may correct themselves as the child grows, while others persist.
Acquired causes primarily involve trauma. Improper anatomical alignment during fracture healing can lead to rotational defects. Neuromuscular diseases, such as cerebral palsy, can create muscle imbalances causing bone twisting. Rarely, infections or tumors affecting bone structure may also lead to deformities.
Symptoms and Clinical Findings
Patients often present with nonspecific complaints. Common symptoms include anterior knee pain, hip pain, and frequent tripping. Observation of inward (intoeing) or outward (outtoeing) foot positioning during gait is a notable finding.
In physical examination, specific angles and tests help localize whether the deformity originates from the hip or tibia.
Fatigue during prolonged standing or running is another common complaint. Conditions like patellofemoral instability may also signal underlying rotational deformity.
Diagnostic Methods: Physical Examination and CT
A definitive diagnosis combines detailed clinical assessment with radiological imaging. While standard X-rays are effective for detecting fractures or angular deformities (such as bowlegs or knock-knees), they are insufficient for measuring rotational abnormalities. Therefore, computed tomography (CT) is the gold standard, with magnetic resonance imaging (MRI) used in specific cases.
CT scans allow for precise measurement of angular relationships between the hip, knee, and ankle joints with millimetric accuracy. The image below demonstrates how rotational measurements are performed on a CT slice.
The diagnostic process can be complex and may overlap with other orthopedic conditions.
The resulting “torsion profile” guides surgical planning. The physician compares measured angles with normative population values to assess deformity severity.
Types of Deformities and Treatment Options
Treatment depends on the patient’s age, symptom severity, and impact on daily life. Mild and asymptomatic cases may only require observation and physical therapy, while severe cases causing pain and dysfunction may necessitate surgery.
The primary goal of surgical treatment is to restore normal bone alignment. This is typically achieved through a “derotation osteotomy,” where the bone is carefully cut and rotated to correct deformity. These procedures, performed within the scope of lower limb deformity surgery, use fixation devices like plates and screws or intramedullary nails.
In certain cases, especially when combined with limb length discrepancies or multi-planar deformities, Ilizarov or external fixator systems may be preferred. These allow gradual correction over time.
Complications and Risk Management
As with all surgeries, rotational deformity correction carries risks, including infection, nerve injury, or anesthesia-related complications. Orthopedically, delayed or impaired bone healing poses significant concern.
Nonunion may require additional interventions; more details can be found on the nonunion surgery page. Malunion, where bone heals in a wrong alignment, may necessitate revision with malunion surgery. Minimizing these risks relies on meticulous preoperative planning (CT analysis) and precise surgical techniques.
Postoperative Period and Rehabilitation
Recovery varies by surgical method but usually involves a period of limited or partial weight-bearing with assistive devices such as crutches. Physical therapy plays a crucial role in maintaining joint mobility and rebuilding muscle strength.
For detailed guidance on post-surgical care and factors supporting bone healing, the post-limb lengthening care resource offers valuable insights, as the principles are comparable. Regular radiologic follow-up confirms bone union and allows safe return to normal activities.
Pediatric Deformities: Rotational Problems in Children
In children, inward (intoeing) or outward (outtoeing) foot positioning is often developmental and may self-correct with growth. Persistent or unilateral deformities beyond certain ages may be pathological.
Children’s bones differ from adults’, requiring tailored treatment approaches that avoid damage to growth plates. Expert evaluation for childhood lower limb deformities is vital for protecting future joint health. Early diagnosis is crucial to prevent lasting gait abnormalities.
Rotational deformity is a complex condition necessitating specialist care. Accurate diagnosis and individualized treatment planning are essential for painless function and mobility.
This content is intended for general informational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare professional regarding any health concerns you may have. Do not delay or discontinue medical treatment based on the information provided here. Medical conditions can vary between individuals, and the most appropriate treatment plan can only be determined after a thorough examination by a healthcare provider.