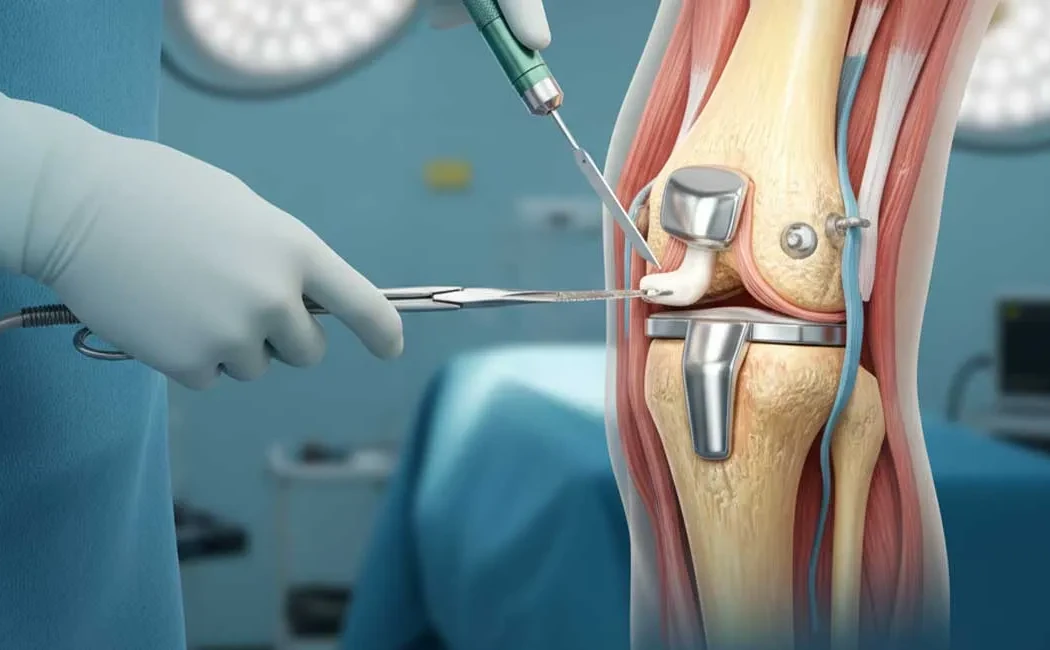
Joint Reconstruction: Solutions for Advanced Damage
Severe damage to the musculoskeletal system can significantly impact individuals' quality of life. Joint reconstruction refers to surgical procedures aimed at restoring the structure and function of joints that have lost their integrity due to trauma, advanced osteoarthritis, infection, or congenital abnormalities. This process is designed to alleviate pain, increase range of motion, and reestablish joint stability. Treatment methods range from osteotomies that preserve the natural joint structure to prosthetic surgeries where damaged surfaces are replaced with artificial implants.
What Is Joint Reconstruction?
Joint reconstruction is more than a simple repair; it is an advanced orthopedic approach aimed at restoring the biomechanics and function of the joint. When cartilage surfaces, ligaments, or bone structure are irreversibly damaged, standard treatments may be insufficient. At this point, reconstructive surgery becomes necessary. The procedure involves comprehensive planning that includes not only the bone tissue but also the soft tissues surrounding the joint.
Reconstruction planning relies on detailed radiological imaging and clinical evaluation, with the goal of enabling pain-free return to daily activities. These surgeries are commonly performed on weight-bearing joints such as the knee and hip but are also successfully applied to the shoulder, elbow, and ankle joints.
When Is Joint Reconstruction Needed?
Indications for joint reconstruction typically involve progressive and structural disorders unresponsive to conservative (non-surgical) treatments. The most common cause is advanced osteoarthritis resulting from aging or trauma. Complete cartilage wear leads to bone-on-bone contact, causing severe pain.
Additionally, pathological conditions like bone tumors may require extensive resections. Losses in bone and joint after tumor surgery are repaired using specialized reconstructive techniques. For more detailed information, see Reconstruction in Bone Tumors.
Congenital or acquired deformities also constitute a significant group necessitating reconstruction. Deformities in the upper extremities can limit hand and arm function. Approaches used in these cases are detailed at Upper Extremity Deformity Surgery. Similarly, corrective procedures addressing leg deformities or discrepancies that affect walking mechanics are reviewed within the scope of Lower Extremity Deformity Surgery.
Prosthetic Surgery: The Core Method of Joint Reconstruction
When natural joint surfaces are too damaged to be preserved, prosthetic surgery (arthroplasty) is considered the gold standard treatment. In this procedure, the worn joint surfaces are surgically removed and replaced with artificial joint components made from durable materials such as metal, ceramic, or polyethylene.
Prosthetic surgery is frequently performed on hip and knee joints. For methods applied in hip osteoarthritis, visit Hip Prosthesis and Coxarthrosis Treatment.
Advancements in surgical techniques and implant technology have increased prosthesis longevity and patient satisfaction. Comprehensive information on hip and knee prosthetic surgeries can be found on the Hip and Knee Joint Prosthetic Replacement and Reconstruction Surgery page. Prosthetic surgery significantly improves patients’ quality of life by enabling pain-free mobility.
Joint-Preserving Surgical Options
Not all joint damage requires prosthetic replacement. Especially in young and active patients, joint-preserving surgeries that maintain the joint’s biological structure are prioritized. These methods aim to correct the load-bearing axis of the joint to reduce stress on damaged areas or to repair cartilage tissue.
Techniques like high tibial osteotomy can alter load distribution in the knee joint, potentially slowing osteoarthritis progression. For detailed discussions on these approaches and their impact on delaying prosthetic surgery, see Can Joint-Preserving Surgeries Delay Knee Prosthesis?.
With proper patient selection, these surgeries can postpone the need for prosthetics by several years, allowing patients to maintain an active lifestyle with their natural joints. Arthroscopic procedures, cartilage grafting, and bone correction surgeries are key options within this category.
Surgical Decision-Making: When Is Each Method Applied?
Choosing the appropriate joint reconstruction method requires a complex decision-making process. Physicians assess variables including patient age, weight, activity level, bone quality, and extent of joint damage. Previous injuries or unsuccessful surgeries also influence planning.
For instance, patients with improperly healed fractures may require corrective surgery for nonunion, which is a prerequisite for successful joint reconstruction. See Nonunion Surgery for more. Similarly, cases where bone healing does not occur adequately are initially treated with Nonunion Treatment Methods.
A multidisciplinary approach is essential in the decision process. Correlating radiological findings with clinical symptoms is key to surgical success. In early stages, joint-preserving methods are preferred; in advanced and extensive damage, prosthetic surgery becomes the primary option.
Recovery and Rehabilitation After Joint Reconstruction
Surgery is only part of the treatment; successful outcomes require comprehensive rehabilitation. Postoperative goals include pain management, wound care, and early mobilization. Physical therapy is crucial to restore joint range of motion and increase muscle strength.
To support recovery and long-term joint health, exercises that protect joint health should be regularly performed. Patient adherence to protocols set by physicians and physiotherapists reduces complication risks.
Recovery time varies by surgery type. Patients generally begin walking the day after prosthetic surgery, while osteotomies or biological reconstructions require more controlled weight-bearing as bone healing progresses.
Potential Risks and Complications
As with any surgery, joint reconstruction carries certain risks. Infection, blood clots (deep vein thrombosis), implant loosening, and nerve injuries are rare but possible complications. These risks are minimized through careful preoperative preparation and strict adherence to sterilization protocols.
Patients at risk for impaired bone healing may benefit from biological treatment approaches to support tissue repair. Smoking, diabetes, and obesity increase complication risk; patient education and preventive measures are essential.
Scientific Sources and Expert Validation
Practices in joint reconstruction and orthopedic surgery are continuously updated based on evolving scientific literature and evidence-based medicine principles. The information presented here is prepared according to guidelines from authorities such as the American Academy of Orthopaedic Surgeons (AAOS), National Institutes of Health (NIH), and the World Health Organization (WHO), as well as latest research. The most accurate treatment information derives from a detailed clinical evaluation by a specialist physician.
The information provided is for general informational purposes only and does not constitute medical advice. It is not intended to replace professional diagnosis, treatment, or guidance. Diagnosis and treatment should be determined only after an in-person consultation with a qualified healthcare professional. Individual clinical conditions vary, and surgical or non-surgical treatments may differ from person to person. The content is based on current scientific research and up-to-date medical practices. Do not delay seeking medical care or consultation with a healthcare professional based on this information.