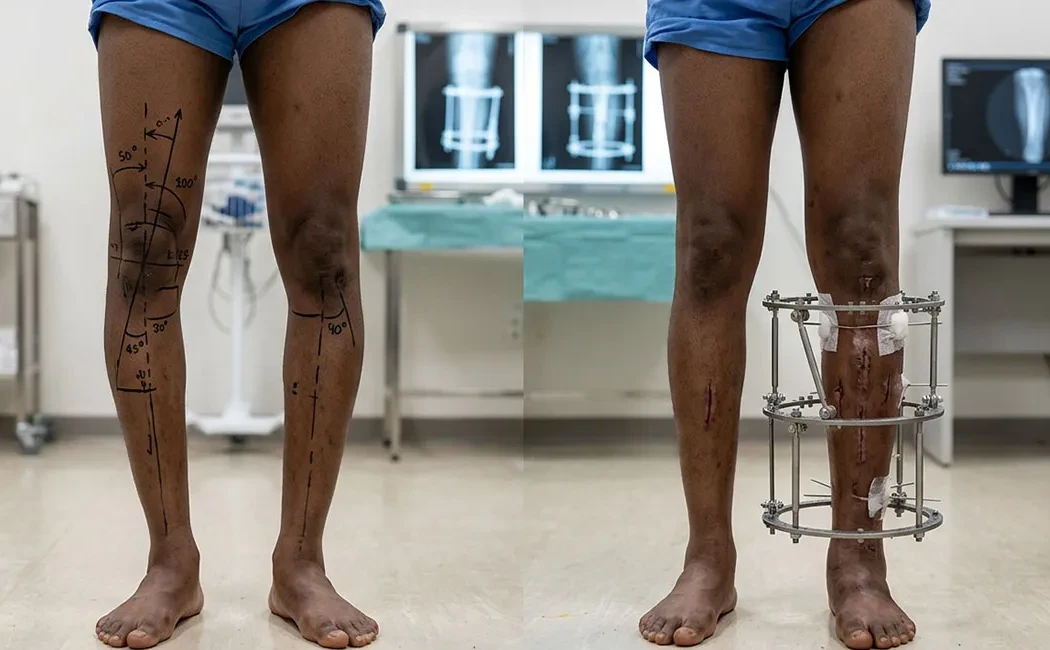
Deformity Surgery: Types, Analysis, and Correction Methods
Structural disorders in the musculoskeletal system can significantly impact an individual’s mobility and quality of life. Deformity surgery is a comprehensive orthopedic specialty aimed at correcting bone curvatures, rotational abnormalities, limb length discrepancies, and joint misalignments. These conditions may arise from congenital anomalies, malunions after trauma, or developmental disorders and require detailed evaluation and personalized treatment plans.
This surgical approach not only corrects bone shape but also optimizes joint load distribution to help prevent future complications such as osteoarthritis. Thanks to modern medical technologies and biological methods, even complex deformities can be treated with high precision.
Introduction to Deformity Surgery
Deformity surgery is among the most technically demanding and meticulously planned areas in orthopedics and traumatology. The primary objective is to restore the anatomical alignment of the affected limb to regain normal function. These procedures address a wide spectrum ranging from simple bone curvature to complex multiplanar deformities and severe bone loss.
Treatment strategies depend on the patient’s age, deformity origin, and severity. Joint-preserving approaches hold particular importance to delay or avoid the need for prosthetic implants. In this context, joint preservation surgeries aim to maintain the patient’s biological joint and represent a core principle in deformity correction.
Types of Bone Deformities
Bone deformities are classified based on their anatomical plane and mechanism. Accurate identification of the deformity type is essential for selecting the appropriate treatment approach. Deformities can be uniplanar or complex, involving multiple planes.
Valgus and Varus Deformities
Angular deformities in the frontal plane are among the most common types encountered. Known as "bow legs" (Genu Varum) or "knock knees" (Genu Valgum), these conditions cause uneven load distribution on the knee joint. In varus deformity, weight concentrates on the inner part of the knee; in valgus, it shifts to the outer part.
Rotational Deformities
Rotational deformities result from twisting of the bone around its longitudinal axis. They might be less obvious visually compared to angular deformities but often manifest as in-toeing or out-toeing gait patterns. These deformities can significantly impact hip and knee joint mechanics.
Limb Length Discrepancies and Shortening
Discrepancies in limb length, where one leg or arm is shorter than the other, lead to both cosmetic and functional challenges. They may be congenital or develop following growth plate injury or trauma. Treatment often involves limb lengthening surgery to equalize limb lengths. For patients interested in aesthetic height increase, cosmetic limb lengthening options are also available.
Deformity Analysis Methods
Successful surgery begins with precise analysis. The correction apex (CORA) and the required correction angle are determined using advanced imaging techniques.
Imaging Techniques: X-ray, CT, MRI
Multiple imaging modalities are combined during diagnosis. Full-length standing X-rays are fundamental to observe weight-bearing axes. Computed Tomography (CT) provides detailed 3D assessment of bony structures, while Magnetic Resonance Imaging (MRI) evaluates soft tissues and cartilage.
Axis Measurement and Angular Evaluation
The most critical phase of deformity analysis involves measuring mechanical and anatomic axes. A line drawn from the hip center to the ankle center allows determining where it passes through the knee joint. The degree of deviation quantifies the severity of the deformity.
Principles of Surgical Correction
Surgical planning is tailored to the location, size of the deformity, and patient expectations. Correction can be achieved acutely (single-stage) or gradually over time.
Osteotomy and Plate-Screw Fixation
Osteotomy involves controlled bone cutting to realign the deformity. The bone is secured in the corrected position using plates and screws, typically applied in acute corrections.
External Fixators and Ilizarov Method
For extensive deformities requiring gradual correction or cases with infection risk, external fixators are employed. The Ilizarov technique is a well-established and effective method in this domain. Particularly in lower limb deformity surgeries, external fixators allow simultaneous correction and lengthening.
Reconstructive Surgical Approaches
Advanced deformities with significant bone loss or severe soft tissue issues necessitate reconstructive surgery, which demands specialized expertise. For instance, upper limb deformity and lengthening surgeries often require microsurgical experience due to delicate nerve and vessel anatomy. Moreover, challenges in limb reconstruction surgery call for a multidisciplinary management approach.
Recovery and Rehabilitation
The postoperative period is key to consolidating surgical success. While bone healing progresses, maintaining joint range of motion and strengthening muscles are priorities. Specialized postoperative rehabilitation programs significantly influence the patient’s return to daily activities.
Technological Advances and Robotic Surgery
Nowadays, computer-assisted navigation and robotic systems minimize errors in deformity correction. Integration of robotic technology in deformity surgery enables surgeons to perform planned correction angles with millimetric precision.
Risks and Complications
As with any surgery, deformity correction carries risks such as infection, nerve injury, or nonunion. Particularly, cases requiring nonunion surgery often involve patients with reduced biological healing capacity. Managing such complications may involve supplementary methods including new biological approaches in bone healing and stem cell therapies.
All information provided is for general informational purposes only and does not constitute medical advice. The content is not intended to replace individual diagnosis, treatment, or professional guidance. Diagnosis and treatment decisions should be made only after an in-person consultation with a qualified physician. Since each patient's clinical situation is unique, surgical or non-surgical interventions may vary accordingly. The information presented is based on current scientific evidence and medical standards.