Hip Replacement Surgery: Advanced Techniques and Durability
The hip joint is one of the body’s primary weight-bearing joints and can lose function over time due to wear, osteoarthritis, or trauma. Hip replacement surgery involves replacing the damaged hip joint with an artificial implant. This procedure aims to reduce pain, improve mobility, and enhance patients' quality of life. Thanks to advances in technology and surgical methods, these operations now have high success rates.
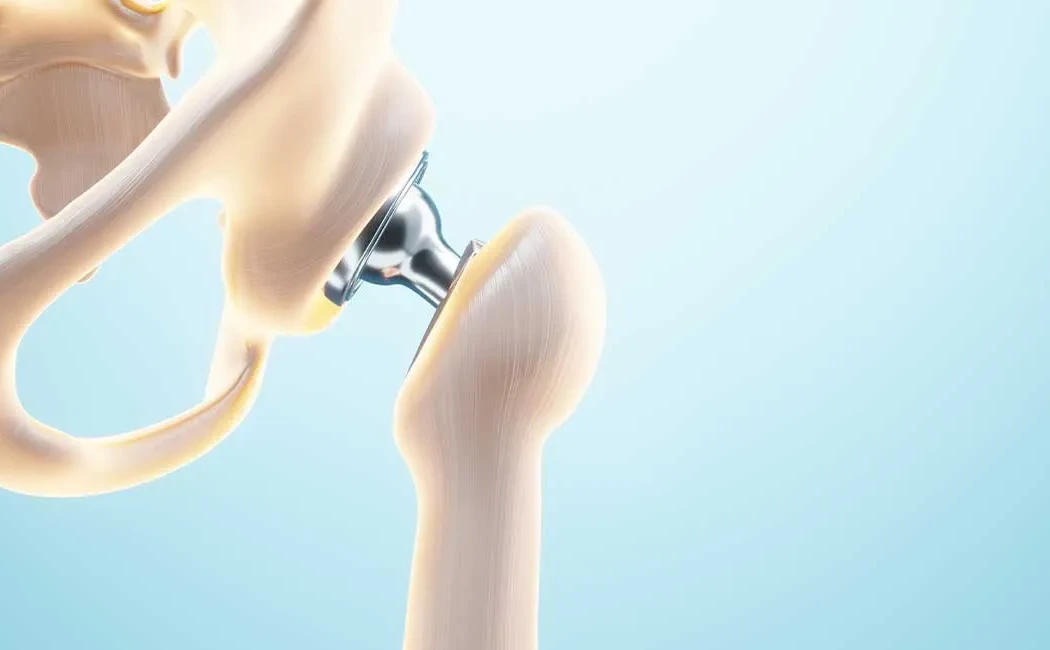
Also known as total hip arthroplasty, selecting implants tailored to the patient's anatomy and lifestyle is crucial. Preoperative planning, surgical precision, and postoperative rehabilitation collectively influence treatment outcomes. Below is an anatomical illustration showing the hip joint structure and implant placement.
Overview of Hip Replacement Surgery
Hip replacement surgery is generally considered when other treatments—such as medication, physical therapy, or joint injections—fail to provide relief. The primary goal is enabling patients to walk pain-free and maintain their daily activities.
What Is a Hip Implant?
A hip implant replaces the femoral head (top part of the thigh bone) and the acetabulum (the socket in the pelvic bone) with artificial components made of metal, ceramic, or durable plastic materials. Designed to mimic natural joint movement, the surgery also ensures balanced soft tissues alongside bone replacement.
Who Is a Candidate?
This surgery is suitable for patients with advanced osteoarthritis (coxarthrosis), hip fractures, or avascular necrosis (bone tissue death). Persistent pain even at rest, limited mobility, and leg length discrepancy contribute to surgical decision-making. Additionally, it can serve as a reconstructive solution for adults with residual deformities from congenital hip dislocation.
Modern Surgical Techniques in Hip Replacement
Medical technology advancements have made hip replacement procedures safer and more comfortable. Beyond traditional methods, several tissue-sparing techniques have been developed to shorten recovery times.
For more information about hip osteoarthritis and replacement surgery, visit Hip Osteoarthritis and Replacement Surgery Details. Our blog on Modern Hip Replacement Surgical Techniques covers technological innovations in depth.
Minimally Invasive Approaches
Minimally invasive surgery involves smaller incisions and minimal damage to muscles and tendons during implant placement. Benefits include reduced postoperative pain, less blood loss, and shorter hospital stays. This technique allows patients to mobilize quicker since muscles are retracted rather than cut. Patient selection criteria are discussed in our article on Current Approaches in Hip Replacement Surgery.
Robotic Surgery and Navigation Systems
Robotic-assisted surgery and computer navigation enable surgeons to position implants with millimeter precision at the optimal angle. Using patient-specific anatomical data, these systems help reduce wear, extend implant longevity, and minimize dislocation risk.
Materials Used in Hip Implants and Their Durability
Implant durability is directly related to the quality and type of materials used. Biocompatible materials currently in use aim to minimize friction and offer long-lasting performance.
Types of Implant Materials
Commonly used materials include metal, ceramic, and highly cross-linked polyethylene.
- Metal-Polyethylene: A widely used and durable combination.
- Ceramic-Ceramic: Offers the lowest friction and highest wear resistance, often preferred for younger, active patients.
- Ceramic-Polyethylene: Has a lower risk of fracture and high durability.
Implant Longevity and Influencing Factors
Modern hip implants can last 15-20 years or longer when placed with proper technique and material choice. For comprehensive information on Hip Implant Durability and Revision Rates, please see our dedicated content. Factors affecting implant life include patient weight, activity level, bone quality, and surgeon experience.
Revision Surgery: When Is It Needed?
Revision surgery involves removing the original implant (primary surgery) and replacing it with a new one. This procedure requires more complex planning compared to the first surgery.
Conditions Necessitating Revision
Revision is typically required due to implant wear, loosening (aseptic loosening), infection, or recurrent dislocations. Periprosthetic fractures (fractures around the implant) may also necessitate revision surgery.
Revision Surgery Process
During revision, the existing implant is removed, and bone defects, if present, are repaired using grafts or specialized metal supports before inserting a new implant. Soft tissue quality and remaining bone stock are carefully assessed. Recovery may take longer than after the primary surgery.
Post-Operative Rehabilitation and Return to Daily Life
Effective rehabilitation complements successful surgery. Patients need physiotherapy-guided exercises postoperatively to regain muscle strength and joint range of motion. The postoperative return to daily life timeline varies individually but generally follows structured protocols.
First Weeks: Mobility and Support
Patients often start walking with assistance on the first day after surgery. During the initial weeks, mobility is supported with a walker or crutches. Careful wound management and use of compression stockings to prevent blood clots are crucial. Following Post-Hip Replacement Care Guidelines reduces complication risks.
Long-Term Rehabilitation
Full recovery and independent walking usually occur within 4-6 weeks, though regaining full muscle strength may take several months. Rehabilitation strategies recommend low-impact activities like swimming and walking while advising against high-impact sports such as running and jumping.
Risks and Complications of Hip Replacement Surgery
As with any surgery, hip replacement procedures carry potential risks that require thorough preoperative assessment and diligent postoperative monitoring.
Surgical Risks
Possible complications include infection, deep vein thrombosis (blood clots), nerve injury, and leg length discrepancy. Antibiotic prophylaxis and strict sterilization are applied to minimize infection risk.
Long-Term Complications
Long-term issues may involve implant wear, loosening, or rarely, fractures around the implant. Problems with bone healing can also arise. Consulting specialists about Non-Union Surgery and Complications is important. Regular follow-up visits allow early detection of potential problems.
In conclusion, hip replacement surgery is a reliable treatment that can significantly improve patients’ quality of life when applied with proper patient selection, modern surgical techniques, and high-quality implants.
This content is provided for informational purposes only and does not constitute medical advice. It is not intended to replace individual diagnosis, treatment, or professional guidance. Diagnosis and treatment should only be conducted following an in-person examination by a qualified healthcare provider. Since each patient's clinical condition is unique, surgical or non-surgical methods may vary accordingly. The information presented is based on current scientific evidence and up-to-date medical practices. Do not delay seeking professional care based on this content. Always consult a licensed healthcare professional for diagnosis and treatment tailored to your specific circumstances.